An Introduction To Diabetic Dermopathy
Diabetic dermopathy is a skin condition that affects up to one-third of people with diabetes. It appears as small, scaly patches on the skin that happens by changes the circulation of blood to the lower extremities. The condition can cause mild discomfort and itching, but it does not pose any serious health risks. Diabetic dermopathy is a common skin condition that affects people with diabetes. It usually appears on the legs as reddish-brown patches or crisscrossed lines. Diabetics are at higher risk of developing this condition due to their impaired circulation and inflammation in the body due to high blood sugar levels.
Causes of Diabetic Dermopathy
1. High blood glucose levels
Over time, sustained high blood glucose levels can lead to diabetic dermopathy. High blood sugar levels can damage the small blood vessels that provide nutrition to the skin and when there is an insufficient amount of these vessels present, it can inhibit the skin’s ability to heal correctly which can eventually form a scaly rash on the skin.
2. Poor circulation
When diabetes reaches an advanced stage, poor circulation of the lower extremities may occur which may in turn affect the skin in those areas of your body. Due to this, rashes may start to appear around this affected area as a result of your body not being able to heal itself as quickly as usual due to poor circulation.
3. Vitamin deficiencies
If someone suffering from diabetes has vitamin deficiencies, then it is more likely for them to develop diabetic dermopathy in some way or another. Vitamin B1 and B12 have been known as important vitamins for healthy skin maintenance and if someone does not have enough of either one in their body then it will become harder for them to heal any cuts or wounds properly which could lead to a possible sign of diabetic dermopathy appearing on their skin.
4. Certain medications
If someone with diabetes is taking certain drugs such as those used in the treatment of tuberculosis or anticonvulsants they are at risk of developing diabetic dermopathy due to how these medication act on their bodily systems and organs—even if they do not suffer from already-high blood sugar levels.
5. Severe trauma/burns
Injuries such as cuts, burns, and other kinds of trauma can be hard for people with diabetes because of due nature of how slower healing rate works with them– leading to possibly having signs of dermopathy appearing around there areas where they got injured or burned so severely it requires medical attention immediately through emergency services.
6. Autoimmune response
Diabetes is an autoimmune disorder and so it’s likely that you will experience episodes where factors like stress, illness, or even things like menstruation could result in your body responding by producing antibodies against its own tissues– including its skin–which may lead towards developing a red scaly rash that looks similar some forms diabetic dermopathy.
7. Improve diet and lifestyle
Finally, regular dietary changes along with reviewing lifestyle habits —regular exercise routine, quitting smoking sugary/processed foods, reducing alcohol consumption – all go hand in hand together with taking prescribed medications regularly are recommended preventative measures against developing diabetic dermopathy altogether.
Symptoms of Diabetic Dermopathy
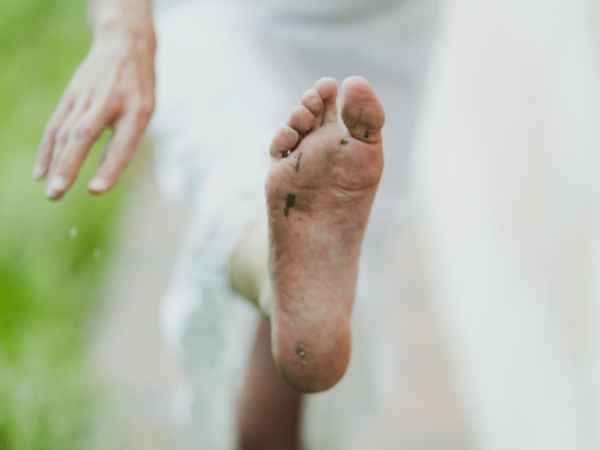
- Discolored patches: Diabetes dermopathy often manifests itself as small, tan, scaly patches of skin. The patches have a spongy texture and usually appear on the legs. They usually don’t cause any other symptoms, but they may be cosmetically inconvenient or irritating for some people.
- Skin thickening: Another symptom of diabetic dermopathy is skin thickening in the affected areas of the legs. This can make it difficult for clothing to fit properly and increases the risk of further injury or infection if not properly cared for.
- Itchiness: Patients may also experience itchiness in the affected area that can range from mild to severe depending on individual cases.
- Blisters: Another common symptom of diabetic dermopathy is blistering which can occur in both the affected areas as well as in other parts of the leg including toes, soles of feet, heels, etc., due to frequent friction caused by ill-fitting shoes or excessive walking/running/standing without proper cushioning/supportive footwear).
- Pain: A less common yet possible related symptom of diabetic dermopathy is pain that has a burning sensation near that areas; if this symptom occurs more commonly than not then medical attention should be immediately sought out since it may indicate complications with diabetes such as circulatory problems like peripheral artery disease (PAD).
- Swelling: Inflammation or swelling near diabetic dermopathy lesions is sometimes experienced by some people due to the long-term presence of abnormal glucose levels in their bodies; this could possibly worsen over time if not caught and managed correctly with regular doctor visits & checkups every few months (or according to doctor’s specific advice).
Treatments of Diabetic Dermopathy
- Topical Corticosteroids: Topical corticosteroids help treat diabetic dermopathy. They are applied as a cream or ointment and can help reduce inflammation and redness in the affected area.
- Laser Therapy: Laser therapy is another treatment option for diabetic dermopathy. It involves using focused beams of light energy that target the damaged areas and helps stimulate skin healing. This therapy can help reduce pain from lesions, minimize their size, and soften the affected skin.
- Photodynamic Therapy: Photodynamic therapy, PDT, is yet another form of laser therapy that treats diabetic dermopathy with minimal side effects or discomfort during treatment. This therapy works by applying a photosensitizing agent to the area before using lasers to target the lesions directly. The treatment reduces both pain and skin discoloration in those with severe cases of diabetic dermopathy.
- Natural Remedies: There are several at-home remedies you can use to help manage diabetic dermopathy including aloe vera, vitamin E oil, honey, turmeric paste, coconut oil, witch hazel extract, and lavender essential oil. These natural remedies provide anti-inflammatory properties which can soothe lesion-affected areas of skin while helping it heal faster due to their moisturizing properties. However, not all natural remedies work for everyone so it’s important to try out different ones until you find one that works best for your individual needs!
- Avoiding Excessive Sun Exposure: Exposure to harsh UV rays from the sun will only worsen symptoms of diabetic dermopathy so if possible try avoiding excessive exposure during peak times like 11 am-3 pm when sunlight is strongest even on cloudy days! Wearing sunscreen over 30 SPF when heading outside can also protect against further irritation and damage caused by UV rays hitting sensitized areas on your body affected by diabetic dermopathy too!
How To Prevent Diabetic Dermopathy?
- Early diagnosis and treatment of diabetes: One of the best ways to prevent diabetic dermopathy is to be conscious about your health, do tests for diabetes early on and initiate treatment if you have it. Control of glucose levels is crucial in preventing further damage to skin cells and tissue so making sure these levels are within the ranges should be a priority.
- Follow a healthy lifestyle: Following a healthy lifestyle such as eating a balanced diet, maintaining a regular exercise routine, avoiding smoking and excessive alcohol usage, and managing stress all play an important role in preventing diabetic dermopathy. Maintaining good overall health as much as possible also helps reduce potential risks associated with diabetes.
- Skincare habits: Proper skincare practices such as avoiding too-hot or too-cold showers/baths, using mild cleansers containing lactic or salicylic acid instead of harsh ones containing bleaches or fragrances that could irritate the skin; keeping the skin hydrated by moisturizing regularly; protecting from environmental toxins (e.g., sunburns); wearing supportive shoes that fit correctly and aren’t too tight; treating any minor issues quickly (eg cuts, scrapes). All these measures help keep skin healthier by reducing chances of irritation which can escalate into complications in people with diabetes-related skin problems like diabetic dermopathy.
- Regular follow-up visits with doctor: Visiting your doctor regularly not only improves awareness about changes happening in your body but gives an opportunity for consultation regarding ongoing concerns like diabetic dermopathy progression or signs thereof observed in time which could potentially become more dangerous over time if not addressed properly while still at early stages and treated accordingly.